New quality improvement project:
Heart attack patients will receive faster treatment.
Only one in ten patients in Northern Norway with an acute heart attack receives thrombolysis quickly enough, before arriving at the hospital, even though they should have had it. A new project in Health North aims to ensure that more patients receive this life-saving treatment within the recommended time.
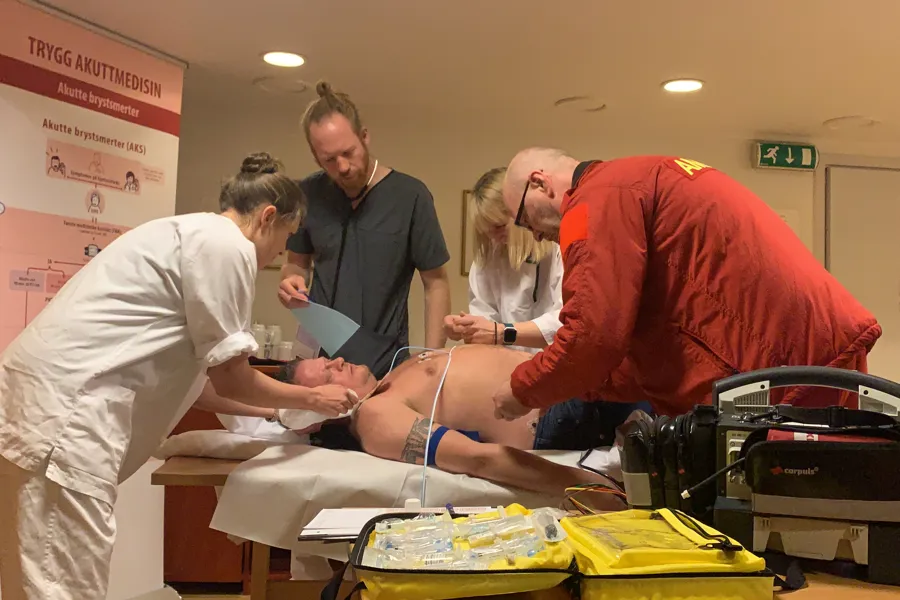
Photo: Mads Gilbert
If you ever call 113 because you or someone nearby is showing symptoms of an acute heart attack, it goes without saying that you want treatment to start as quickly as possible. And there is little time to lose:
— When a blood clot causes an acute blockage of a coronary artery in the heart, we know that time is a critical factor. Especially the first 120 minutes. It is the emergency treatment you receive during this time that can determine how many cells die in the heart muscle and how extensive the damage from the heart attack will be. In the worst case, it can be fatal, explains chief physician at the University Hospital of Northern Norway (UNN), Mads Gilbert.
Together with advisor in the Coordination Section at UNN, Stein Widding, they lead the project “Safe Emergency Medicine in the North,” which is managed from UNN, Health North.
The project aims to increase the proportion of patients with acute heart attacks (STEMI patients) who receive pre-hospital thrombolysis in Northern Norway within the nationally recommended times.
Updated information on Safe Emergency Medicine
Worst in the country
Thrombolysis means dissolving the blood clot (thrombus) that acutely blocks the coronary artery and leads to the heart attack. For simplicity, thrombolysis is often referred to as “plumbo” because it is an effective way to dissolve the blood clot and reopen the coronary artery. This restores the vital blood supply to the heart muscle.
Receiving thrombolysis pre-hospital means that you receive treatment before you arrive at the hospital, perhaps in the ambulance or at home where you are having the heart attack. According to national guidelines, patients with acute heart attacks should receive pre-hospital thrombolysis when it is more than 120 minutes to the nearest hospital with 24-hour advanced cardiac imaging and coronary artery reopening (PCI). In Northern Norway, many acute patients with heart attacks will not be able to reach such acute PCI treatment because the population is dispersed and has a long way to the nearest PCI hospital.
— Nationally, two out of ten heart attack patients receive pre-hospital thrombolysis in time before they arrive at the hospital. In Health North, however, it is only one in ten who receives it – even though they should have. This means that far too few patients receive it at the right time, and now we are the worst in the country according to national quality data, points out Stein Widding.
For the patient, faster thrombolysis means reduced mortality and a lower risk of heart failure after the heart attack for those who survive.
— In other words, it is vital time for the patient that we must not waste, believes Mads Gilbert.
Faster treatment with pre-hospital thrombolysis is in line with the recommendations from the Norwegian Heart Attack Register and national goals. To improve in this area, the Safe Emergency Medicine project has set a goal that patients who need it should receive thrombolysis treatment where they are, within the first 20 minutes after the first physical contact with healthcare personnel who can take an ECG and make a diagnosis. If they cannot reach a PCI hospital within 90 minutes after the ECG diagnosis is made.
Launching checklists
20 minutes is a short time. Achieving such a time target requires that the emergency medical teams in the region, with participants from municipal health services, ambulance services, air ambulance services, and the 12 acute hospitals in Health North, have the same situational awareness and follow the same plan. Therefore, a new, evidence-based common action plan (algorithm) and common checklist for working with these time-critical patients have been developed. Regardless of whether you are a nurse in a nursing home, an ambulance worker, a GP, an AMK operator, or healthcare personnel in a hospital, everyone should work according to the same plan to save vital patient time and quickly make the right decisions together.
The Safe Emergency Medicine project organises day courses in teamwork with common situational awareness, common action plans, and common time targets. During the course, healthcare personnel practice realistically on collaborating quickly, effectively, and safely. To avoid misunderstandings in a time-critical work situation, they train on using checklists, which is entirely new.
— Checklists are mandatory in all aviation to prevent forgetfulness and misunderstandings that can cost lives. Checklists are now also being used with good results in all Norwegian operating theatres to ensure safe anaesthesia and surgery, says Mads Gilbert.
Stein Widding points out that there is also an HSE aspect to this. Common action plans, time targets, and checklists make it safer for individuals to be on duty. The risk decreases that healthcare personnel with acute responsibilities become uncertain or forget important things when time is of the essence.
— Checklists make us safer, he says.
Delighted with funding
The programme has already been “rolled out” in the Health Community of Troms and Ofoten over the past couple of years.
— How was the course received by the participants?
— It has been received with great enthusiasm! We have received feedback that this contributes to the professionals working faster and more safely with greater assurance for the patient. Among the approximately 500 who have participated so far, there are particularly two recurring themes: Finally, we have had time to train together to become good, and finally, there has been agreement on how the workflow and timetable should be, says Mads Gilbert.
Recently, the Safe Emergency Medicine project received two million kroner in support from the infrastructure funds for quality register fields.
— For us, it was like Christmas Eve and 17 May all at once when we received the message that our application was granted. This is also a project that Health North has welcomed, says Gilbert.
— We have spent time applying for funds, so we are very pleased with the help we have received from the National Service Environment at the Centre for Clinical Documentation and Evaluation (SKDE), adds Stein Widding.
The project is planned to run for two years.